Health equity has been recognized as a core dimension of quality for more than two decades, beginning with the Institute of Medicine Report (Crossing the Quality Chasm, 2001). However, adding health equity as a quintuple aim is too much in terms of aims and too little in terms of priority. The preceding paper by Dzau et al offers further support for health equity being a national priority. The authors articulate cogent arguments for health equity improvement being a national aim. Adding health equity as the quintuple aim, with its linkage to measurement, transparency, and reimbursement, will help sustain attention to persistent inequities plaguing our health systems and communities. We are coupling that approach with the training and engagement of trusted community voices such as Black church leaders, hair-dressers and barbers, and community-based pharmacists. At the Center for Sustainable Health Care Quality and Equity (SHC) we are implementing quality improvement education programs for clinical teams serving people of color, helping them close gaps in vaccination, diabetes management, evidence-based heart failure treatment, and other conditions characterized by disparities in care and outcomes. Strategies that helped make vaccines more available, such as true community engagement, delivery of services in the community, and attention to social determinants of health, will not continue. But my colleagues and I fear that the urgency to address equity will fade as the pandemic recedes. COVID certainly spotlighted health inequities. Providers need to focus their efforts on assessing and prioritizing the clinician experience.ĭownload the Quadruple Aim ebook to learn more about each Aim and how HealthStream has mapped multiple solutions to each of these critical issues.įrom solutions with a focus ranging from clinical development and reimbursement to quality and performance management, HealthStream is dedicated to improving patient outcomes through the development of healthcare organizations' greatest asset: their people.I applaud the authors' call for making health equity the fifth rail of the "quintuple" aim, including measurable and transparent reporting, consideration of systemic contributing factors, and tying it to reimbursement. healthcare organizations are plagued by staff dissatisfaction, burnout, staff disconnection with leadership, and care providers who suffer from a loss of meaning in their work. Improving the clinician experience – U.S.Clearly, there is room for improvement when it comes to improving healthcare outcomes in the U.S. 
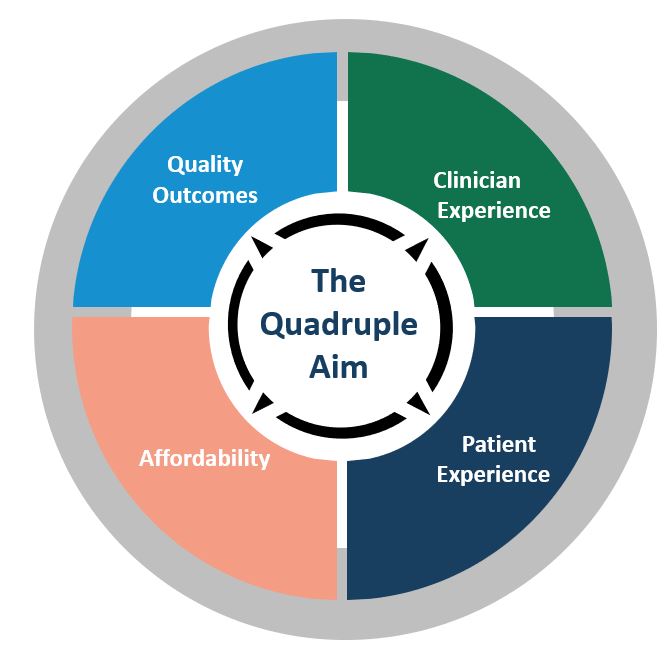
healthcare, we perform extremely poorly in terms of life expectancy, the suicide rate, chronic disease burden, obesity rate, and highest rate of avoidable deaths, to name just a few statistics among many that are regrettable. Improving healthcare outcomes – Despite the high cost of U.S.It's no wonder that reducing costs has become such a healthcare imperative. The disastrous impact of the pandemic leaves the financial outlook for healthcare extremely bleak. Reducing costs – Even prior to the COVID-19 pandemic, many hospitals and other healthcare organizations were operating on super-thin margins, in the vicinity of 3.5%, which were expected to be negative by 2025.At the same time, healthcare leaders understanding that better patient experience of care is strongly correlated with positive clinical outcomes and improved profitability. Enhancing the patient experience – Patient experience has become an important focus because patients are demanding better service and also want to be more involved in their own healthcare decision-making.healthcare.Its chapters, based on each of the four aims, include: This blog post is the first in our blog series based on the HealthStream ebook, The Quadruple Aim, that explores this effort to improve and reform the provision of U.S. 
Department of Health and Human Services (HHS), the Centers for Medicare and Medicaid Services (CMS), and other institutions, has been augmented with an additional goal, improvement of the clinician experience, creating what is now commonly known as the "Quadruple Aim." Four strategies focused on improving healthcare outcomes for all involved in care Several iterations later, the framework for making healthcare better settled in 2008 on three goas-improving the patient experience of care, improving population health, and reducing per capita cost, an approach developed by the Institute for Healthcare Improvement (IHI), known as the "Triple Aim." Since then, this strategy, adopted widely by the U.S. 
healthcare system's radar since at least 1999, when the Institute of Medicine (IOM) published To Err is Human: Building a Safer Health System. Improving healthcare quality has been firmly on the U.S.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
